Bloomberg reports that several insurers are seeking double-digit percentage increases in 2019. Since implementation of the Affordable Care Act in 2014, rates in the Midwest have skyrocketed. In the case study below, this small employer has seen their rates increase 86% in 5 renewal cycles.
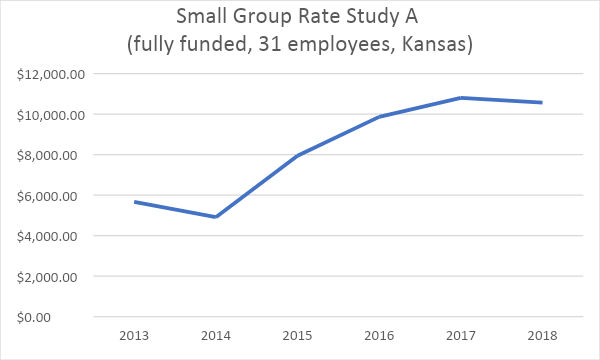
Initially, this group saw a small decrease in premium by changing from a grandfathered plan to an ACA plan. But since the change, their costs have doubled. How much does a small business have to increase its top line revenue to counter the extraordinary increase to its bottom line expenses?
While the ACA was touted as a solution to eliminating waste in the system thus making healthcare affordable, the American Institute for Economic Research published this Executive Brief outlining how significant the impact would be on small fully funded group plans. Group plans that are/were grandfathered and self-funded were among those least likely to be impacted. Interestingly, the AIER estimated 230 million people to see “little or no noticeable change” in premiums.
What impact did the ACA have on your group premiums? Employers who have seen price hikes like the group in our study may benefit from self-funding . Below is an example of a small business taking advantage of a self-funded plan.
